Posterior tibial tendon dysfunction (PTTD)
WHAT IS IT?
Posterior tibial tendon dysfunction (PTTD) is an over stretching of the posterior tibial tendon in the foot which generally occurs after long term overuse related inflammation and degeneration of the tendon. The tibialis posterior muscle/tendon has a major role in supporting the medial arch of the foot and therefore its dysfunction can lead to flattening of the feet.
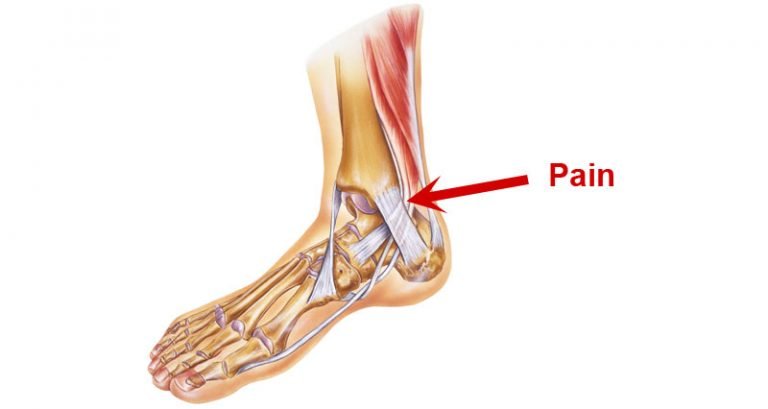
The posterior tibial tendon is a fibrous cord that extends from a muscle in the leg. It descends the leg and runs along the inside of the ankle, down the side of the foot, and into the arch. This tendon serves as one of the major supporting structures of the foot and helps the foot to function while walking.
When there is post-tibial tendon disfunction, the tendon does not function to hold up the arch, resulting in flat feet. This can lead to heel pain, arch pain, plantar fasciitis &/or heel spurs.
It is often referred to as “adult-acquired flatfoot” because it is the most common type of flatfoot developed during adulthood. Although this condition typically occurs in only one foot, some people may develop it in both feet. It is a progressive condition, which means it will keep getting worse if not treated early.
CAUSES
Overuse of the posterior tibial tendon is frequently the cause and symptoms usually occur after activities that involve the tendon, such as running, walking, hiking, or climbing stairs.
Post-Tib Tendon dysfunction occurs when the muscle is overused and the tendon that connects the muscle to your bone is strained and eventually weakens. Years of over-pronation (flat feet) can also lead to posterior tibial tendon dysfunction. If you keep overusing the muscle, damage to the tendon builds up and tendonitis develops. At first the pain or swelling may come and go quickly, but eventually the problem may become more permanent.
SYMPTOMS
PTTD is often referred to as a progressive condition meaning that the symptoms change the longer the condition is present. Staged symptoms can include:
Stage 1 Pain, tenderness or swelling on the inside of the shin, ankle or foot (along the course of tendon)
Stage 2 Flattening of the medial longitudinal arch of the foot. At this point the foot and toes can begin to turn outward and the ankle rolls in.
Stage 3 The arch flattens even more and the pain shifts to the outside of the foot. The foot itself becomes rigid and flexibility/movement of the foot lessens. Tibialis posterior aching and muscle fatigue increases. At this point the tendon has deteriorated considerably and arthritis often develops in the foot. In more severe cases, arthritis may also develop in the ankle.
TREATMENT
Because of its progressive nature, it’s best to see your podiatrist as soon as possible as early treatment is vital. If treated early enough, your symptoms may resolve without the need for surgery. Such treatments may include:
- Orthotic devices or a brace to give your foot and arch the support it needs
- Immobilisation. Sometimes periods of rest are required and if needed a cast or Camwalker/ moonboot is worn to immobilise the foot and allow the tendon to heal. You may also be advised to completely avoid all weight bearing for a while.
- Physical therapy. Ultrasound therapy, heat therapy and strengthening exercises may help rehabilitate the tendon and muscle following immobilisation, These therapies will differ from case to case.
- Medications. Nonsteroidal antiinflammatory drugs, such as ibuprofen, help reduce the pain and inflammation in some cases.
- Shoe modifications or support shoes, such as athletic footwear (sneakers) or orthopedic shoes may be required.
- RICER during periods where active inflammation is present.
