Fungal Toenail Treatment
What is Fungal Nail?
Our toenails are subject to the constant presence of bacteria and fungi (picture the environment inside a shoe).
Fungal toenails, also known as onychomycosis is one of the most common nail conditions that we see as podiatrists. It is a slow growing fungus that is commonly the same fungus that causes tinea.
Fungal infections usually occur underneath the nail and begin at the end of the nail (where it gets trimmed) and are caused by a spreading of a fungus under the nail plate and into the nail bed. Fungi grow in the warm, moist environment inside socks and shoes. Fungal nail infection can also appear as a white, powdery discoloration on top of the nail.
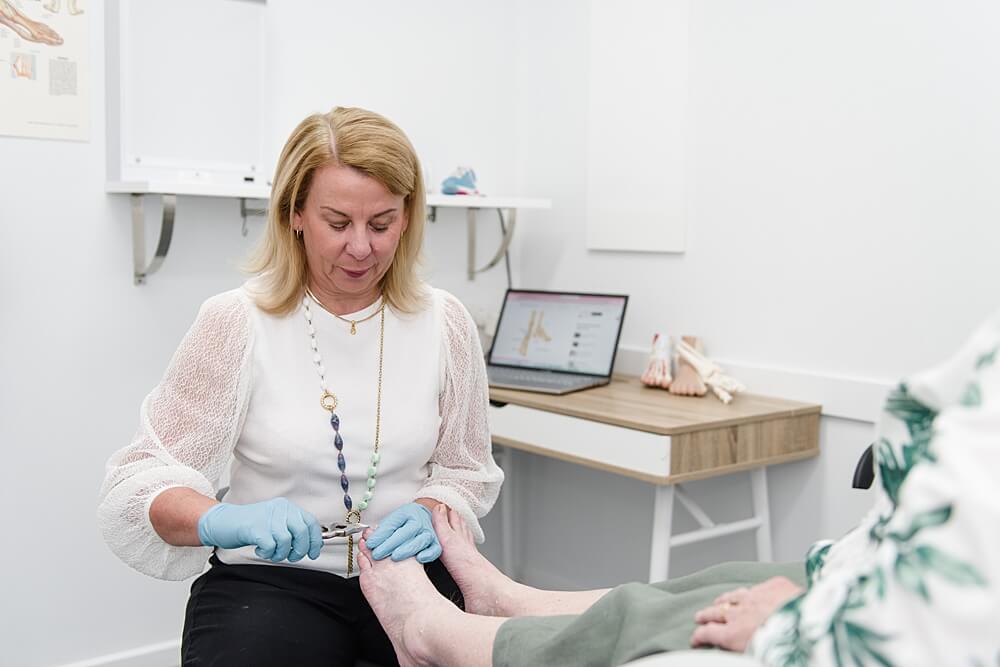
Symptoms
The most common symptoms of fungal toenails infections include:
Thickened nails
The affected nail may become thicker than usual, making it difficult to trim.
Discoloured nails
The nail may become yellow, brown, or white, and may have spots or streaks.
Brittleness
The nail may become brittle, crumbly, or ragged, making it easier to break.
Distorted nail shape
The nail may become distorted, and its shape may change, such as curving or bending.
Foul odour
The infected nail may emit an unpleasant odour.
Separation from the nail bed
In severe cases, the infected nail may separate from the nail bed, causing pain and discomfort.
Pain and discomfort
The affected nail may become painful or uncomfortable, especially when walking or wearing shoes.
It’s important to note that not all nail changes are due to fungal infections, and other conditions such as psoriasis or injury can cause similar symptoms. If you suspect you have a fungal nail infection, it’s best to see a healthcare professional for a proper diagnosis and treatment plan.
Causes
Toenail fungus is often picked up in public gyms, showers, and swimming pools as fungal organisms thrive in these warm, damp environments where they can infect the toenails through small cuts in the skin around the nails or through the opening between the nail and nail bed.
Factors that can lead to developing Fungal Nails include:
Trauma, allowing entry into the nail or nail bed
Trauma to the nail or nail bed can create small openings that allow fungi to enter and infect the nail. For example, a nail injury such as a cut or puncture wound can provide a pathway for fungi to enter the nail. Similarly, frequent use of artificial nails or other nail products can cause trauma to the nail and increase the risk of fungal infection.
Abnormal pH level of the skin
The normal pH of the skin is slightly acidic, which helps to protect against fungal and bacterial infections. However, certain factors such as excessive sweating, frequent exposure to water, and the use of alkaline soaps can disrupt the skin’s pH balance, making it more susceptible to fungal infections. Additionally, skin conditions such as eczema or psoriasis can also affect the skin’s pH and increase the risk of fungal infections.
Not drying off feet thoroughly after exercise or bathing
Fungi thrive in warm, moist environments, and failing to dry the feet properly after exercise or bathing can create an ideal environment for fungal growth. This is particularly true in the areas between the toes, where moisture can accumulate and create a breeding ground for fungi.
Wearing tight enclosed shoes that don’t allow feet to breathe
Wearing tight, enclosed shoes can create a warm, damp environment that promotes fungal growth. This is especially true if the shoes do not allow for adequate ventilation, trapping moisture and sweat in the shoes and on the feet.
Individuals with compromised immune systems
People with compromised immune systems, such as diabetics and the elderly, are more susceptible to fungal infections due to reduced immune function. In addition, poor circulation and nerve damage associated with diabetes can make it harder for the body to fight off infections and increase the risk of fungal nail infections.
Treatment Options for Fungal Nails
It is recommended you see your podiatrist, if you suspect an infection before the toenail fungus spreads.
Treatments include:
Prescribed oral antifungals
Oral antifungal medications are often prescribed by our podiatrists to treat fungal nail infections. These medications work by killing the fungi causing the infection. They are usually taken for several weeks or months and may be more effective than topical antifungal medications.
Topical antifungals
Topical antifungal medications are applied directly to the infected nail and surrounding skin. These medications work by stopping the growth of the fungi causing the infection. While they are generally less effective than oral antifungal medications, they can be a good option for mild to moderate infections.
Debridement/nail removal
In some cases, the infected part of the nail may need to be removed to allow for effective treatment of the underlying infection. This can be done through debridement, which involves removing the affected nail tissue, or through partial or complete nail removal.
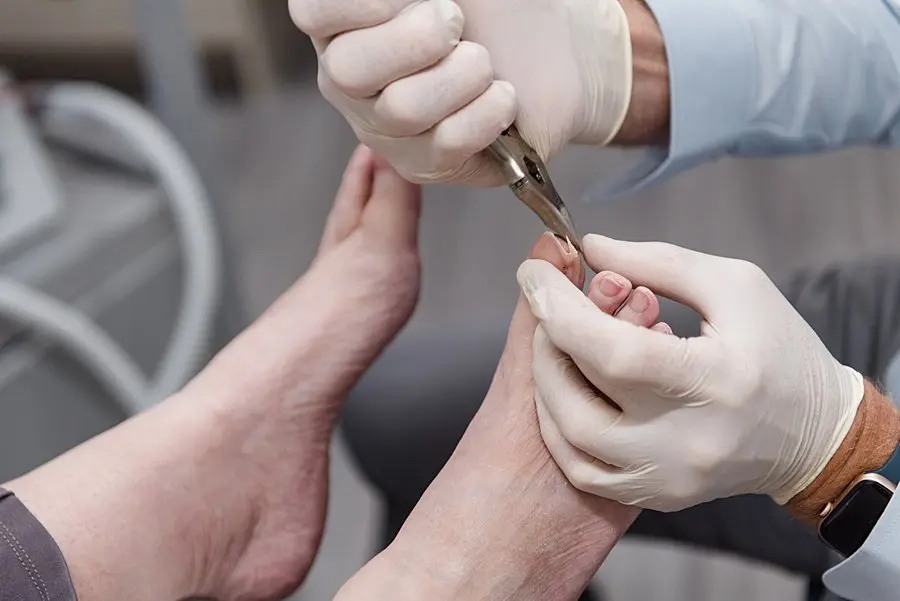
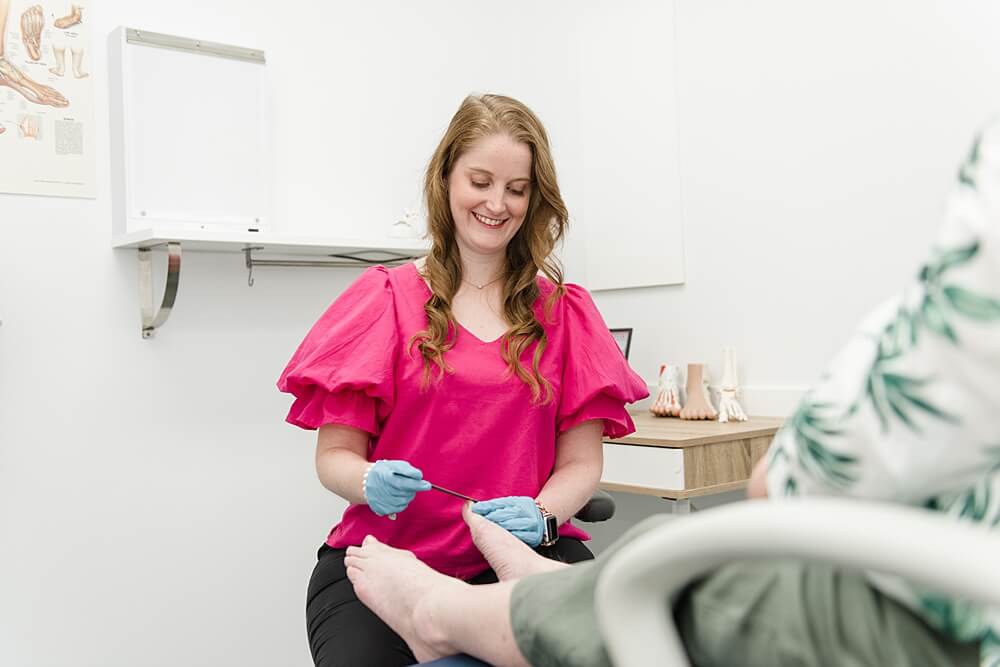
Podiatrist tools
Podiatrists have tools to reduce the thickness of the fungal nail so that topical medication can be more easily absorbed, thus providing more comfort to the patient this will also allow for better penetration of topical antifungal medications. This can be particularly helpful for patients with thick or difficult-to-treat fungal nail infections.
Complications
If left untreated, fungal nail infections can cause several complications, including:
- Pain and discomfort: The infection can cause pain, discomfort, and swelling in the affected area, making it difficult to walk or perform daily activities.
- Nail deformities: The nail may become thickened, discoloured, and brittle, and may even begin to separate from the nail bed, causing a permanent deformity.
- Spread to other nails and body parts: Nail infections can easily spread to other nails on the same foot or hand, as well as to other parts of the body, such as the skin or groin area.
- Bacterial infection: A nail infection can make the nail more vulnerable to bacterial infection, which can cause further complications and may require antibiotic treatment.
- Reduced quality of life: Nail infections can be unsightly and embarrassing, leading to reduced self-esteem and quality of life. They may also cause feelings of self-consciousness or anxiety in social situations.
It’s important to seek treatment for fungal nail infections to prevent complications and to improve the appearance and health of the affected nail.
Prevention
You can take several steps to prevent fungal nail infections, including:
- Wash your feet regularly with soap and water, and dry them thoroughly, especially between your toes.
- Choose shoes and socks made from breathable materials that allow air to circulate around your feet.
- If you are prone to fungal infections, you may want to use an antifungal powder or spray in your shoes and on your feet.
- Fungal infections can spread from person to person, so it’s important to avoid sharing items like nail clippers or socks.
- Wear sandals or flip-flops in public places like communal showers, locker rooms, and swimming pools to reduce your risk of exposure to fungal infections.
- Try to avoid injuring your nails, and if you do sustain an injury, clean and disinfect the area to prevent infection
Frequently Asked Questions
How long does it take for an infection to clear up?
Is it possible for the infection to come back after treatment?
How much does it cost to treat a fungal nail infection?
Additionally, the cost may vary depending on whether the treatment is covered by private health insurance or Medicare. It’s best to consult with a healthcare provider to get a more accurate estimate of the cost of treatment for a fungal nail infection in Australia.
Can wearing nail polish make a fungal nail infection worse?
Can a fungal nail infection be contagious?
How long should I wait to apply nail polish after treating a fungal nail infection?
Always Consult A Trained Professional
The information in this resource is general in nature and is only intended to provide a summary of the subject matter covered. It is not a substitute for medical advice and you should always consult a trained professional practising in the area of medicine in relation to any injury or condition. You use or rely on information in this resource at your own risk and no party involved in the production of this resource accepts any responsibility for the information contained within it or your use of that information.
