Diabetes and Your Feet
How can diabetes affect your feet?
- Elevated blood glucose levels associated with Diabetes can cause damage to nerves and arteries in legs and feet.
- This can lead to outcome of poor blood supply in the feet, loss of sensation and diabetic foot ulcers.
- Changes to the feet often happen slowly, and can easily go undetected for years if not checked regularly by your health professional.
- If you suffer from bunions, hammer toes, difficulty shoe fitting and/or heavy callus and restricted joints, you are at higher risk of diabetic foot complications.
How can we help?
- We can advise you on how diabetes may be affecting your feet and work with you to create a plan to protect your feet.
- We assess and monitor any vascular, neurological, biomechanical, dermatological changes and assess footwear to help you avoid complications and injury.
- Our diabetic assessments are conducted depending on your personal risk factors – at a minimum annually to monitor any changes in the feet.
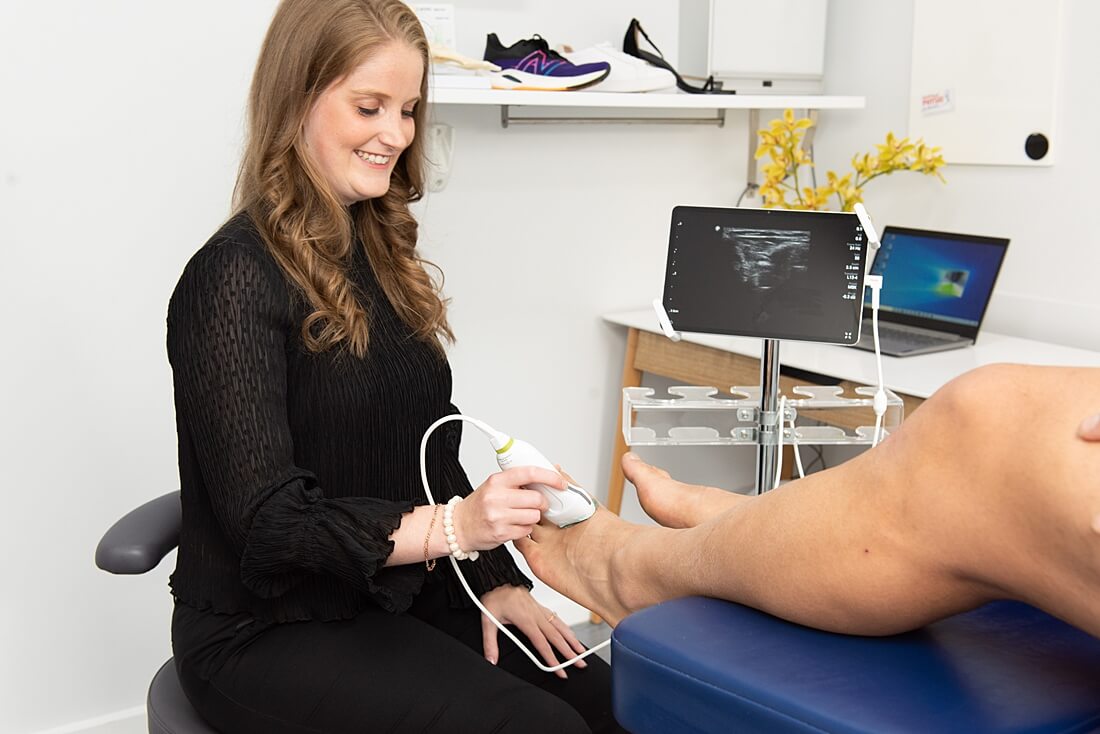
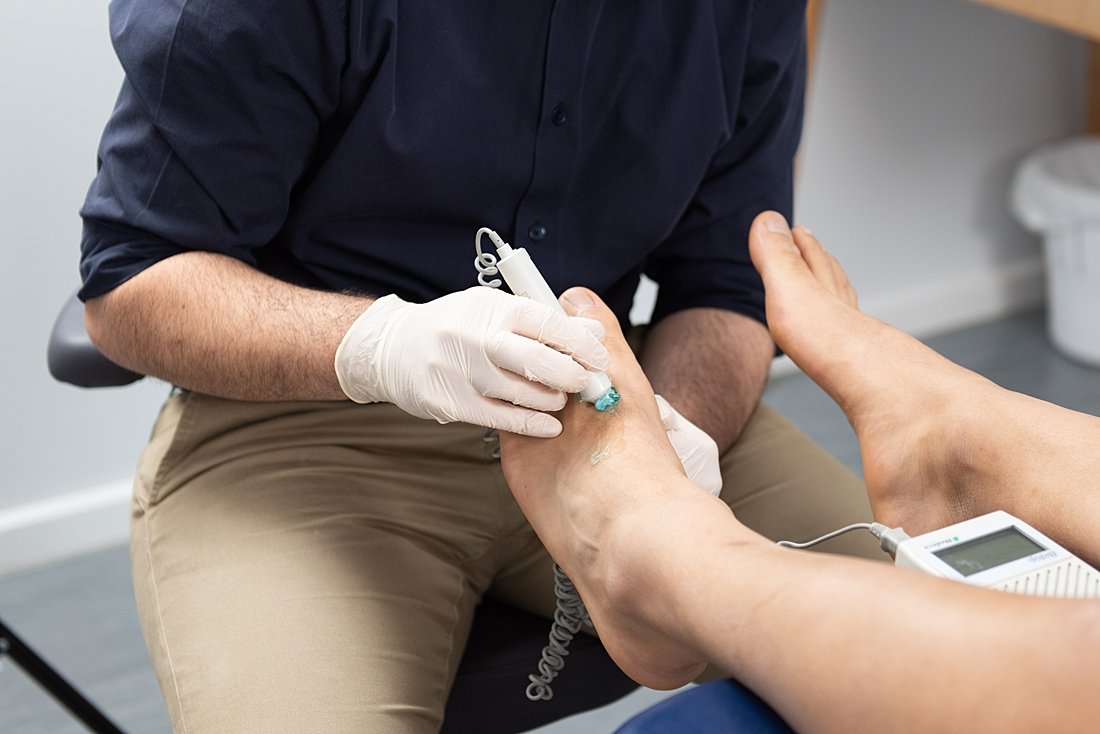
- We use a Doppler ultrasound to enable us to assess the volume and rate of the blood flow to your feet and helps in the identification of blood clots, vessel narrowing or any other abnormalities.
Diabetic Foot Assessments
Diabetes is a common health condition in the community. Here in Australia 280 people are diagnosed with diabetes every day. Many people with diabetes live a healthy and fulfilling life. However, Diabetes can have some complications, and the feet can be particularly at risk because they contain tiny blood vessels and nerves.
The main risk factors for patients are:
Peripheral neuropathy (loss of protective sensation)
Peripheral neuropathy can lead to ulceration, and if left untreated, sepsis, osteomyelitis, and amputation. Regular check-ups are crucial for high-risk patients to assess numbness and protective sensation, structural or gait changes. Regular checks can detect minor loss of sensation and treat minor problems such as corns and calluses before chronic ulceration occurs.
Peripheral arterial disease (reduced blood flow)
Peripheral arterial disease delays wound healing and can cause wounds if severe. Cuts and abrasions can lead to major infections in patients with reduced blood flow. If left untreated this can lead to hospitalisation and possible amputation.
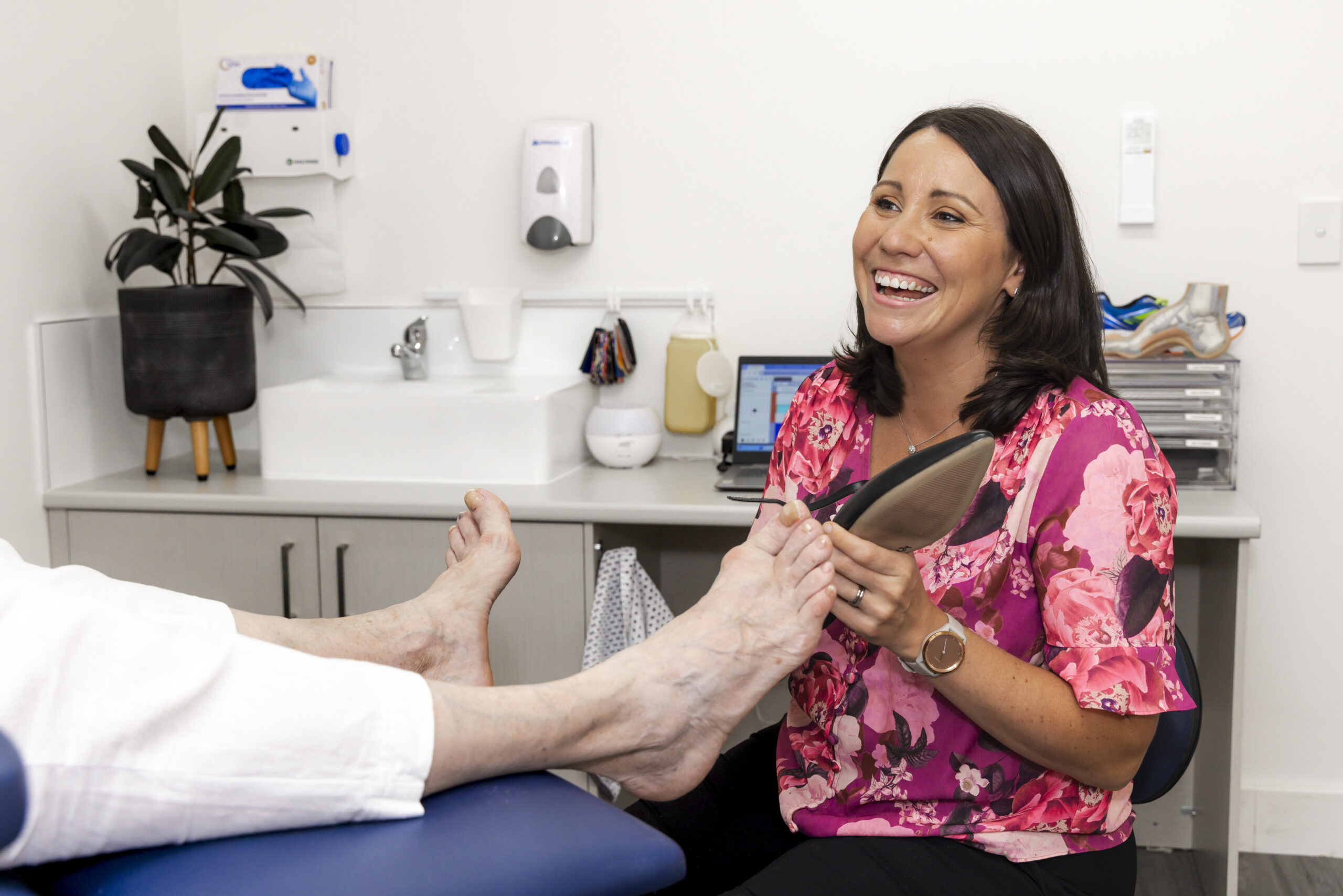
Structural deformity
Bone deformity and joint mobility problems resulting from conditions such as bunions, hammertoes, prominent bones, restricted joints and arthritis can lead to high pressure areas within the foot. These areas can predispose you to corns, callus and are the most common spots for diabetic ulceration. Footwear plays a big role in this area and we know that 90% of foot ulcerations are predisposed by ill-fitting footwear.
ASSESSMENTS
Patients with diabetes should have a foot examination by their podiatrist at least once a year to assess and monitor risk. If you are classified as high risk due to ulceration or amputations in the past, medical history or foot deformity, then more regular assessments will be advised. We will do an individual plan for your individual circumstance. The foot examination should assess protective sensation, foot structure, biomechanics, vascular status, skin integrity and footwear choices. Good foot care can help to reduce the risk of disease-related foot complications.

Always Consult A Trained Professional
The information in this resource is general in nature and is only intended to provide a summary of the subject matter covered. It is not a substitute for medical advice and you should always consult a trained professional practising in the area of medicine in relation to any injury or condition. You use or rely on information in this resource at your own risk and no party involved in the production of this resource accepts any responsibility for the information contained within it or your use of that information.
