SHIN SPLINTS TREATMENT
WHAT ARE SHIN SPLINTS?
Shin pain is commonly referred to as shin splints and pain is often felt along the shin bone (tibia – the large bone in the front of the lower leg). The muscles, tendons and bones become inflamed and pain can last anything from hours to days, to weeks and even months.
Shin pain is a common injury suffered by athletes, particularly those participating in running and jumping-based sports, e.g. basketball, netball, football. It is characterised by pain in and around the tibia (shin bone) in the lower leg and usually occurs as a result of a sudden increase in the frequency, duration and/or intensity of activity.
Shin pain can be categorised into 3 types.
- Medial Tibial Stress Syndrome
- Medial tibial stress syndrome is the most common type of shin pain. Pain is usually felt along the lower medial two-thirds of the tibia.
- Inflammation of the muscle where it attaches to the shin bone from strain causes pain in the area. Sometimes the area can be hot or red, although where the pain is reported is usually the primary diagnostic indicator. The pain usually worsens with running and jumping and improves with rest.
- Tibial Stress Fracture
- A stress fracture of the tibia is painful, particularly on weight-bearing and can also be felt at night in bed. The pain is usually focused on one specific area of the tibia. Tibial stress fractures are caused by muscle pulling on the tibia, repeatedly, eventually causing the bone to crack.
- Anterior Compartment Syndrome
- Shin pain of the lower leg caused by swelling in the shin area caused by swelling or inflammation of the muscles that compress the nerves and blood flowing to the feet and lower leg.
- The pain usually onsets after some time exercising and subsides when exercise stops.
SIGNS AND SYMPTOMS
The signs and symptoms of shin splints include the following:
- Pain in the front of the lower leg along the shinbone
- Tenderness, soreness or swelling inside the shin
- Pain that develops gradually over time, often during or after exercise
- Intense pain at the beginning of exercise that gradually subsides
- Pain that returns or continues for some time after exercise
- Pain that is relieved upon rest, but returns when exercise is resumed
- Pain that is sharp or dull, and may be accompanied by a sensation of tightness or fullness in the calf
If you experienced any of these symptoms, it may be necessary to consult with your podiatrist to determine the best course of treatment.
WHAT CAUSES SHIN SPLINTS?
Like most overuse injuries, shin pain may develop gradually over a period of time. Often the early signs are ignored with those continuing the activities causing the problem.
Some of the causes may include:
Abnormal biomechanics
When there is an imbalance or dysfunction in the biomechanics of the foot and lower leg, it can lead to excessive stress on the shinbone and surrounding tissues. This can occur due to overpronation (when the foot rolls inward excessively) or oversupination (when the foot rolls outward excessively).
Training methods
Overuse of the lower leg muscles due to sudden increases in training intensity, frequency, or duration can cause shin splints. Additionally, running on hard surfaces, running downhill, or engaging in activities that require frequent stops and starts can increase the risk of shin splints.
Training surfaces
Running on hard surfaces, such as concrete, increases the impact on the lower leg, which can cause shin splints. Similarly, running on uneven surfaces or surfaces with poor shock absorption can also contribute to shin splints.
Footwear
Wearing shoes that lack proper support, such as worn-out shoes or shoes with inadequate arch support, can increase the risk of shin splints.
Poor flexibility
Tightness in the calf muscles or Achilles tendon can increase the stress on the shinbone and surrounding tissues, leading to shin splints.
Low bone density
Individuals with low bone density are at a higher risk of developing stress fractures in the shinbone.
Poor diet
Nutritional deficiencies, such as low vitamin D or calcium levels, can lead to weaker bones, which can increase the risk of stress fractures and subsequent shin splints.
TREATMENT FOR SHIN SPLINTS
As with most acute soft tissue injuries, treating shin splints consists of the RICER protocol – rest, ice, compression, elevation and referral. RICE protocol should be followed for 48 – 72 hours, with the aim to reduce the bleeding and damage within the soft tissue.
The No HARM protocol should also be applied – no heat, no alcohol, no running or activity modification, and no massage. This will ensure decreased bleeding and swelling in the injured area.
At Highett Podiatry we will institute a personalised treatment regime for you, including:
Pain relieving treatments
One way to treat shin splints is to take pain relieving treatments such as ice therapy, non-steroidal anti-inflammatory drugs (NSAIDs), and rest can help to reduce pain and inflammation associated with shin splints.
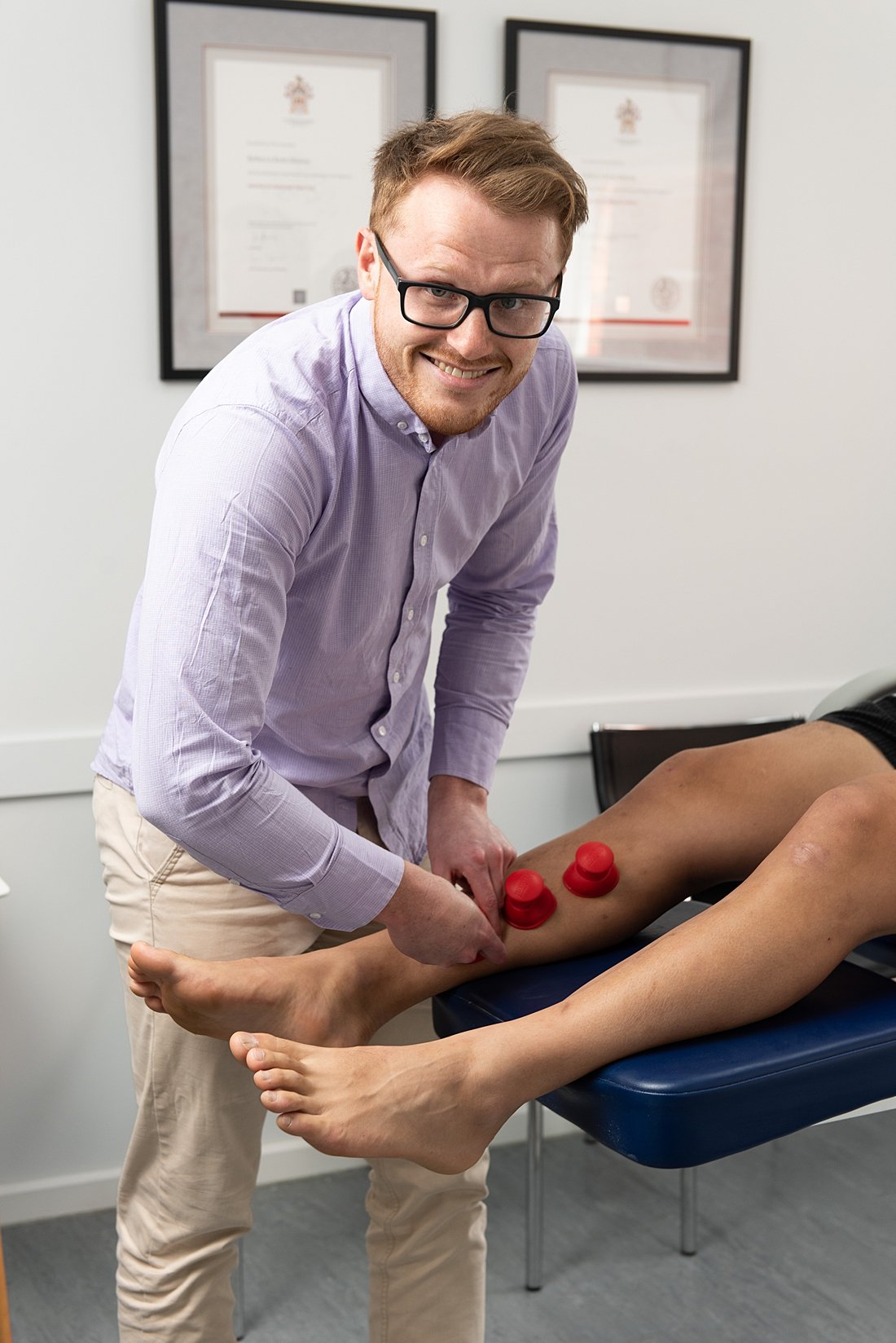
Soft tissue therapy
Soft tissue therapy including therapeutic ultrasound, massage, dry needling, taping, and cupping can help to reduce muscle tension and improve circulation, allowing for better healing of the affected area.
Correction of biomechanical issues
Correction of biomechanical issues such as flat feet, overpronation, and muscle imbalances can help to address the root cause of shin splints and prevent reoccurrence.
Orthotics
Orthotics such as splint, arch supports or custom-made shoe inserts can help to provide additional support and improve alignment of the feet and legs.
Footwear recommendations
Footwear recommendations such as wearing shoes with good cushioning and support can also help to reduce impact on the lower legs and prevent shin splints.
Training and rehabilitation advice
Other ways to cure shin splints is to do training and rehabilitation advice such as gradually increasing activity levels, cross-training with low-impact exercises, and modifying training surfaces can help to prevent overuse injuries and allow for proper recovery.
Specific stretches for flexibility
Specific stretches for flexibility, such as calf stretches and ankle mobilisation exercises, can help to improve range of motion and prevent muscle tightness that can lead to shin splints.
Specific strength and muscle conditioning program
Specific strength and muscle conditioning programs, such as exercises to strengthen the calf muscles and improve ankle stability, can help to prevent reoccurrence of shin splints.
Return to activity plan
Return to activity plans that gradually increase intensity and duration of exercise can help to prevent re-injury and allow for proper healing.
It is recommended to participate in low impact activities such as swimming, cycling and deep-water running to keep fit whilst recovering from shin pain.
Please call us on 95553044 for a comprehensive assessment and treatment plan to manage your shin pain, or alternatively you can book online by clicking the link below.
